Patient OmbudsmanOmbudsman 2021/22
Making connections
Supporting a better health system for everyone



Patient Ombudsman’s message
Resilience, reassurance and change. Those are the three driving factors behind the work we do.
Read Craig Thompson’s message

Patient Ombudsman’s message
I am pleased to be sharing my second annual report as Patient Ombudsman and highlighting the dedication and hard work my office engages in to ensure fairness in the delivery of health care in Ontario.
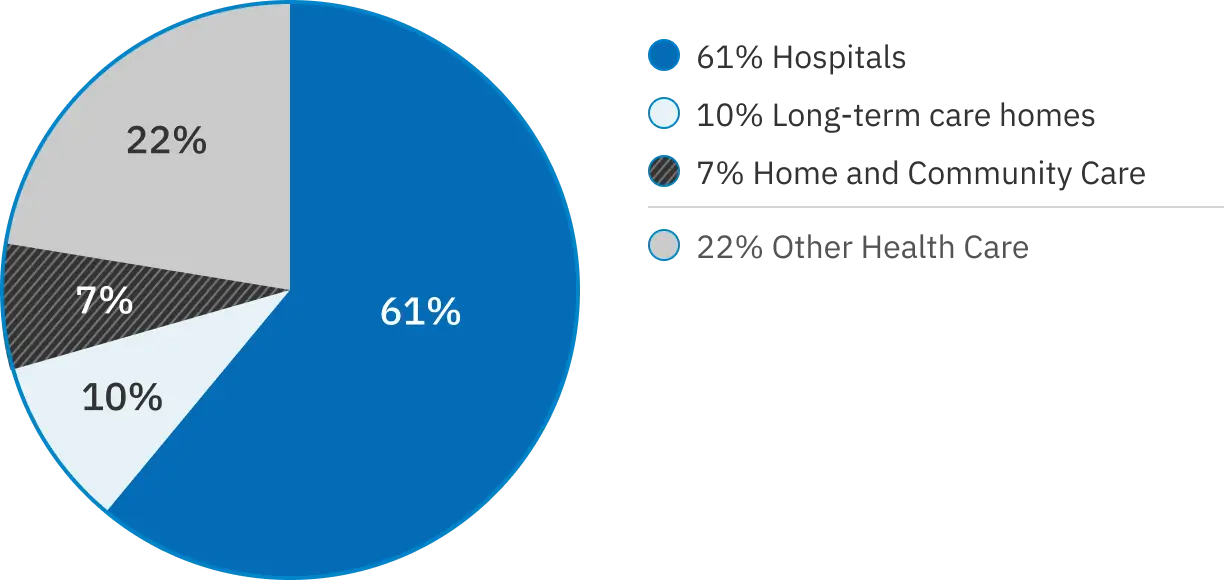
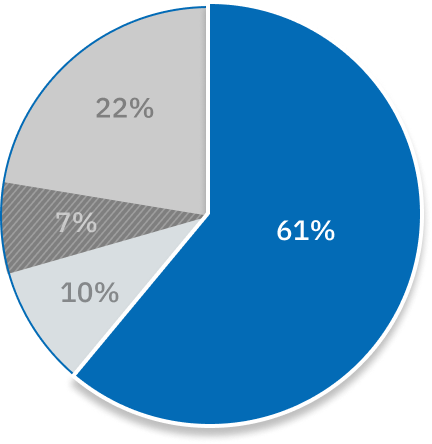
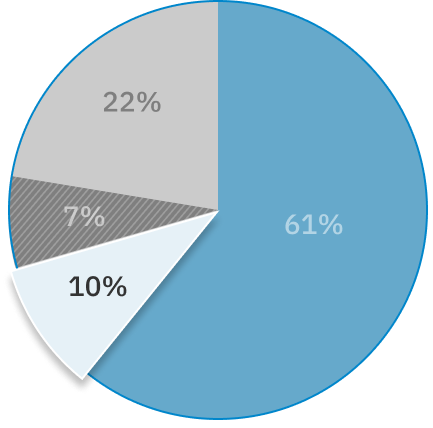
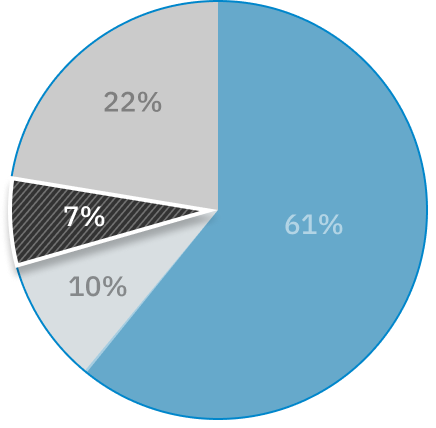
As the office that receives and helps resolve complaints about Ontario’s public hospitals, long-term care homes, and home and community care services, Patient Ombudsman saw a substantial increase in complaints following the start of the COVID-19 pandemic in 2020. Like many, we hoped there would be an eventual “return to normal,” but as we entered 2021-22, the effects the pandemic brought about are still being felt throughout the health care system and continue to be reflected in the complaints we receive.
An Exhausted System
Like many of you, we are seeing signs of strain, stress and a system doing its very best to persevere in the face of ongoing challenges. While complaints about COVID-19 itself represent fewer of our total complaints in 2021-22 than in recent years, the pandemic has exposed existing vulnerabilities in our health system that are seen in the rising number of complaints that touch on lack of access to care, lack of adequate staffing, and a general sense of fatigue. The complaints we received last year demonstrated the strain that everyone – both patients and care providers – is under. More and more we are seeing complaints that touch on issues of sensitivity, caring, courtesy and respect.
Many health organizations continue to report staffing shortages due in part to illness, which results in longer wait times in hospital and delays in accessing home care, as well as restrictions to visitation due to illness and outbreaks in long-term care homes.
This secondary strain COVID-19 is placing on the health care system presents in other ways as well. Studies carried out during the first wave of the pandemic showed COVID-19 increased the use of psychiatric drugs (such as sleeping pills or antidepressants) in long-term care homes to help manage residents when the home is short staffed, or due to increased distress in long-term care residents due to social isolation and loneliness. We know from our own COVID special reports that long-term care home residents and their caregivers noted a decline in resident health and well-being and that a lack of visitation due to COVID-19 contributed to significant stress and decline.
Moving Forward
Our sixth year in operation was busy, not only due to an increase in complaints, but also the release of our second and third special COVID reports, which looked at the later waves of the pandemic and experiences from long term-care home residents and their caregivers; the completion of our investigation into fair and transparent billing practices; as well as significant work on our first systemic investigation into long-term care homes during the first wave of the pandemic.
Patient Ombudsman continues to adapt to changes to the health care system, including changes that were made to the home and community care services regulation in spring 2022 that expand our jurisdiction effective September 1, 2022.
Resilience and Reassurance
Though our health care system continues to face challenges, I feel there is always opportunity to make connections and work for positive change.
Throughout 2021-22, I was able to meet with key stakeholders, including patients, residents, caregivers and staff of health sector organizations, to talk about the role Patient Ombudsman plays bringing together everyone who has a stake in our health care system and demonstrating how complaints are an opportunity for improvement. While many health organizations are under immense stress, they are still eager to learn how they can proactively address patient, resident, and caregiver concerns to make health care experiences more positive.
My team is equally dedicated to continuing its important work as an agent of positive change in our health system. I know many of our frontline staff are buoyed when they know they were able to help achieve a fair resolution, or when a resolution can’t be reached, that they were able to lend a supportive ear and talk patients and caregivers through some of the most difficult times of their lives.
Bringing forward concerns about a negative health care experience takes courage. We are grateful to the patients, residents, staff and caregivers who have reached out to us to discuss these concerns as it benefits us all. For our part, we continue to listen to and learn from Ontarians and work for fairness in health care.
Sincerely,
Craig Thompson,
Patient Ombudsman
What Patient Ombudsman does
We champion fairness for everyone, and work to ensure more positive health care experiences for all Ontarians.
Read our vision and mission
What Patient Ombudsman does
Our Vision
To be a trusted champion for fairness and to influence positive change in Ontario’s health care system.
Our Mission
We facilitate resolution and investigate complaints involving health sector organizations, without taking sides, and make recommendations to improve experiences for all Ontarians.
As set out in the Excellent Care for All Act, 2010, Patient Ombudsman’s role is to receive, respond to and help resolve complaints from current or former patients or their caregivers about their care or experiences with public hospitals, long-term care homes and home and community care support services organizations. We work with all sides to try and find a fair resolution.
Patient Ombudsman believes that resolutions are best achieved at the point of care. As an impartial office of last resort, Patient Ombudsman can help when patients and caregivers have not been able to resolve their complaint directly through the internal complaints process with the health care organizations.
Some matters may be outside of Patient Ombudsman’s jurisdiction. We cannot offer direct help if the complaint is about the treatment decisions of health care professionals (such as a doctor or nurse), an organization outside our jurisdiction (such as a walk-in clinic or retirement home) or if the complaint is part of another proceeding (such as, a lawsuit or coroner’s inquest). When the complaint is outside our jurisdiction, we can navigate patients and caregivers to someone who can help.
Patient Ombudsman Team
The office of the Patient Ombudsman is made up of a team of approximately 20 individuals with a diverse set of skills and backgrounds. The core frontline team includes Early Resolution Specialists and Investigators who are skilled at listening, analyzing and applying the principles of fairness to concerns. The frontline team is also knowledgeable about the health care system and the options available to patients and caregivers when their concerns fall outside our mandate.
What do we mean by fairness
Many ombuds offices use the principles of fairness when looking at the issues and circumstances that make up a complaint or concern. When working to resolve a complaint, Patient Ombudsman tries to ensure that the resolution process itself is fair for everyone involved.
Our Fairness Triangle outlines a set of principles or considerations that Patient Ombudsman uses when analyzing a complaint and testing if a resolution is fair. Our Fairness Triangle is based on a tool developed by Ombudsman Saskatchewan and was developed in close consultation with our frontline complaints team as well as patients, caregivers, health care patient relations specialists and others to address our unique role in resolving and investigating complaints. This tool has been helpful in providing transparency to health care organizations about how Patient Ombudsman approaches complaints and what we are looking for in the organization’s responses.
Evolution of the Office
The Changing Nature of Complaints
Patient Ombudsman’s sixth year of operation was a time of growth, change and new challenges.
As we grow and evolve as an office, Patient Ombudsman has started to collect a body of work – including data, reports, and recommendations – of patient and caregiver experiences that allows us to better shine a light on issues that continue to challenge and strain our health care system.
Complaints that included concerns related to COVID-19
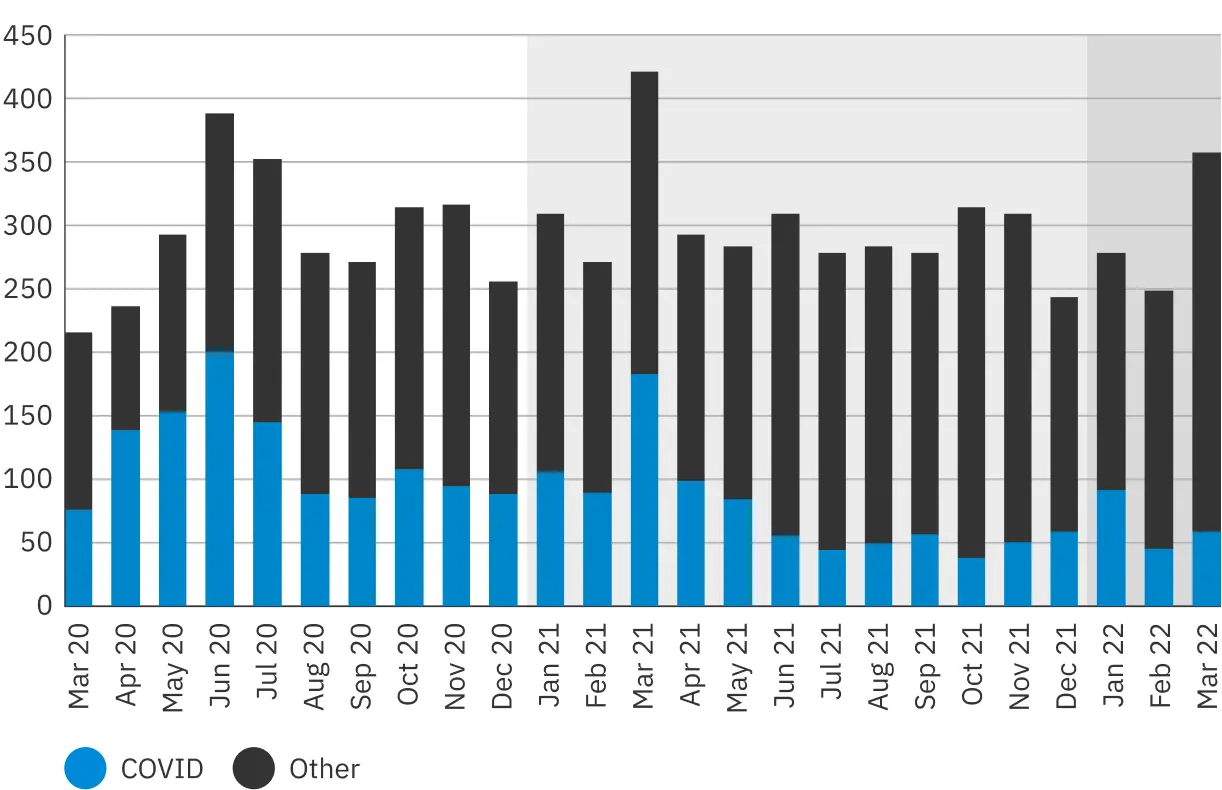
The COVID-19 pandemic had a dramatic effect on both the volume and focus of the complaints Patient Ombudsman received in 2020/21. While the number of new complaints remained high in 2021/22 – and continues to grow – the nature of the complaints changed. Patient Ombudsman continued to receive complaints about challenges with restrictions on visiting in hospitals and long-term care homes, vaccination, testing and infection control but in lower volumes.
The pandemic, however, continued to be an important factor, exposing and aggravating long-standing stresses on the health care system that affect patients’ and caregivers’ experiences.
Special reports
In addition to our complaints work, our second and third special COVID-19 reports were released in August and December 2021, respectively, and provided important context to patient, caregiver, and long-term care home residents’ experiences due to the pandemic.
Putting patient and resident experiences at the centre of these reports helped highlight the ways in which the pandemic affected care and increased loneliness, depression, and decline. In those reports, our office made recommendations regarding the essential role of caregivers, the need for clear communication in a crisis, necessary supports for the health care workforce, and considerations that health organizations should make when implementing restrictions to visitation.
Patient Ombudsman also finalized an investigation into fair billing practices, which included recommendations to protect patients from financial abuse.
Spotlight issues
Lessons We Can Learn
Patient Ombudsman monitors the complaints we receive to identify emerging issues. Our “Spotlight” stories shine a light on the kinds of cases we receive, how we achieve resolutions, and where health sector organizations can look for opportunities to improve patient and caregiver experiences.